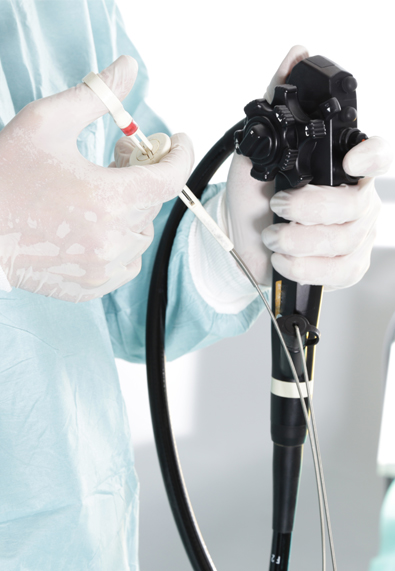
Update on Scope Reprocessing
Recently the FDA issued a statement from Jeff Shuren, M.D., J.D., Director of the Center for Devices and Radiological Health, on updated rates of duodenoscope contamination from preliminary postmarket data. According to the statement:
“The FDA has been involved in an extensive and ongoing effort to prevent patient infections associated with the transmission of bacteria from contaminated duodenoscopes. As part of these efforts, the FDA ordered all U.S. duodenoscope manufacturers—Olympus, Fujifilm, and Pentax—to conduct two postmarket surveillance studies to determine whether health care facilities were able to properly clean and disinfect the devices.”
“These studies are critical to our efforts to evaluate whether the devices’ instructions for reprocessing (e.g., cleaning and disinfecting) are being adequately adhered to by health care facilities, are properly preventing transmission of infections, or should be re-evaluated.”1
In the fall of 2013, the FDA first learned about the association between multi-drug resistant bacteria (e.g., CRE) and duodenoscopes. Upon further investigation, it became clear that these cases of infection were occurring despite confirmation that device users were following proper manufacturer cleaning and disinfection or sterilization instructions. 2
In August of 2015 the FDA sent warning letters to several medical device manufacturers whose scopes had been blamed for spreading deadly CRE bacteria.
The devices were used in hundreds of thousands of procedures each year. In the warning letters the FDA said that the companies failed to validate their cleaning instructions for use (IFUs) to ensure that the devices could be thoroughly cleaned. 3
"Over the last several decades, we have seen an increase in the number of failures or lapses in flexible endoscope reprocessing as well as patient infections reported," said Naomi Kuznets, PhD., vice president and senior director of the AAAHC Institute for Quality Improvement. "The costs of these failures include patient morbidity, mortality, pain and suffering, and decreased productivity, as well as legal, testing and treatment costs." 4
On February 26, 2018, the FDA, Centers for Disease Control and Prevention (CDC), and the American Society for Microbiology (ASM), together with other endoscope culturing experts, released voluntary standardized protocols for duodenoscope surveillance sampling and culturing. Hospitals and health care facilities that utilize duodenoscopes may, in addition to meticulously following the manufacturer’s reprocessing instructions, now take these additional steps to further reduce the risk of infection and increase the safety of their duodenoscopes. 5
In December, 2018 the FDA issued yet another safety communication dealing with the on-going problems, challenges and patient infection risks associated with scopes that cannot be completely cleaned during reprocessing. This most recent communication dealt with additional steps that scope users should take to further enhance their reprocessing. Specifically:
“In today’s safety communication, in addition to supplemental reprocessing measures, we are also recommending that hospital staff carefully inspect a component of the duodenoscope that is difficult to clean, called the elevator recess, and to repeat cleaning if any soil or debris is visible.
However, it has become clear that following the manufacturer’s reprocessing and maintenance instructions, while critical, is not sufficient to avoid all infections associated with the use of duodenoscopes. That is why the FDA has also been working with developers on new product designs, including disposable components. Technological advances in product design hold promise to reduce the risk of contamination and enhance patient safety. Interim results from the sampling studies indicate higher-than-expected contamination rates after reprocessing, with up to 3 percent of properly collected samples testing positive for more than 100 colony forming units of low concern organisms that are unlikely to cause serious infections (but an indication of a reprocessing failure) and an additional 3 percent of properly collected samples testing positive for “high concern” organisms. These are bacteria more often associated with disease, such as E. coli or Staphylococcus aureus (staph).”5
As all of the FDA communications and warnings point out, the on-going problem with scopes centers on the failure to validate cleaning instructions for use (IFUs) to prove that those IFUs actually work. In the absence of cleaning IFUs that have been validated by independent laboratory testing using AAMI and FDA testing protocols, reprocessing personnel can be following the manufacturer’s IFUs and still be returning contaminated scopes.
The documented patient harm caused by scopes who’s IFUs have not been validated is just the tip of the iceberg. According to the CDC, over 30,000 patients die annually from surgical infections. Many of these deadly infections are caused by contaminated instruments who’s cleaning IFUs have never been validated. Without independent laboratory validation of a device’s cleaning IFUs, reprocessing personnel do not have the ability to provide clean, sterile, moisture-free instruments for every patient, regardless of how hard they try.
- https://www.fda.gov/NewsEvents/Newsroom/PressAnnouncements/ucm628096.htm
- https://www.fda.gov/MedicalDevices/ProductsandMedicalProcedures/ReprocessingofReusableMedicalDevices/ucm454630.htm
- https://www.fda.gov/ICECI/EnforcementActions/WarningLetters/2015/default.htm?Page=6
- AAAHC website https://www.aaahc.org/institute
- https://www.fda.gov/NewsEvents/Newsroom/PressAnnouncements/ucm628096.htm
March 15, 2019
5 view(s) 
